Boletín administrativo: 2026-05-005 Recordatorios
Fecha: 1 de mayo de 2026
Los temas tratados en este boletín administrativo aplican a:
Proveedores profesionales y de centros
- Certificación de datos de proveedores y actualización de información demográfica.
- Ediciones médicamente improbables (MUE): actualización del sistema de edición de reclamaciones y recordatorio de facturación.
- Exámenes de diagnóstico de cáncer de mama.
Solo proveedores profesionales
- Certificación del CAQH - Recordatorio.
- Requisitos de facturación e informe de unidades de factores de coagulación para la hemofilia: actualizaciones del sistema de edición de reclamaciones.
- Nuevos graduados que solicitan unirse a la red.
Solo proveedores de centros
A menos que se indique lo contrario, si tiene alguna pregunta relacionada con la información de este boletín, comuníquese con su asesor para proveedores o visite capbluecross.com/wps/portal/cap/provider/pec-look-up e ingrese su NPI o ID tributaria para identificar su punto de contacto designado en Capital Blue Cross.
Proveedores profesionales y de centros
Certificación de datos de proveedores y actualización de información demográfica
- CHIP
- EPO
- FEP PPO
- HMO
- Medicare Advantage HMO
- POS
- PPO
- Tradicional e Integral
- Medicare Advantage PPO
PUNTO CLAVE: Los cambios demográficos de los proveedores deben enviarse mediante las herramientas de mantenimiento de proveedores y mantenimiento de instalaciones de Capital Blue Cross en nuestro portal web para proveedores, y NO a través de la herramienta de administración de datos de proveedores de Availity. También se les recuerda a los proveedores que deben revisar y validar sus datos una vez cada 90 días.
Proceso de certificación:
La Herramienta de mantenimiento de proveedores mostrará la fecha de vencimiento y permitirá a los proveedores revisar todos los datos requeridos de acuerdo con la Ley de Asignaciones Consolidadas de 2021. Una vez revisados los datos, tienes dos opciones:
- Certificar que los datos son precisos.
- No se requiere ninguna acción adicional.
- Certificar, pero hacer las actualizaciones correspondientes.
- El proveedor tiene 3 días hábiles para volver a ingresar y actualizar la información.
La certificación debe realizarse como se describe; de lo contrario, el sistema no permitirá a los proveedores continuar con otras actividades diarias ni actualizaciones de la herramienta.
Los grupos grandes o los sistemas de salud deben continuar utilizando el proceso de lista vigente directamente con Capital.
Proceso de cambio de datos demográficos:
Nota importante: En la página de inicio de Availity Essentials, es posible que vea un menú desplegable de la Herramienta de administración de datos de proveedores de Availity. Los cambios introducidos en esta herramienta NO se envían a Capital Blue Cross. En cambio, siga las instrucciones detalladas a continuación para asegurarse de estar en la página de Espacios del pagador (Payer Spaces) de Capital Blue Cross.
- Inicie sesión en Availity. En la página de inicio, seleccione Capital en el menú desplegable Espacios del pagador (Payer Spaces).
- Haga clic en la pestaña Applications (Solicitudes).
- Desde allí, elija Maintenance Provider (Mantenimiento del proveedor) para enviar los cambios de datos demográficos del profesional electrónicamente, o seleccione Facility Maintenance (Mantenimiento del centro) para enviar los cambios de datos demográficos del centro electrónicamente.
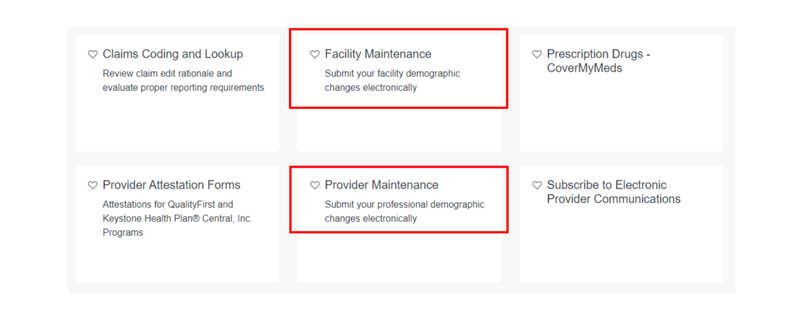
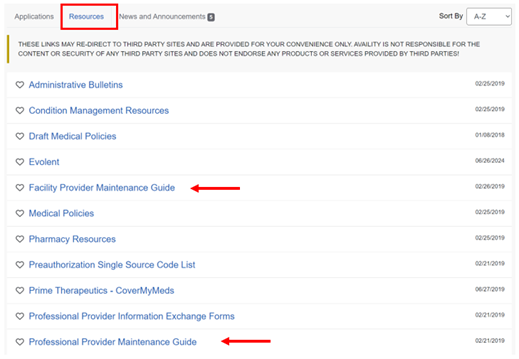
Puede encontrar guías útiles para completar actualizaciones demográficas en la pestaña Recursos.
Nota para los proveedores participantes de Medicare Advantage: Según 42 CFR § 422.111(b)(3), los Centros de Servicios de Medicare y Medicaid (CMS) exigen que las organizaciones de Medicare Advantage tengan directorios de proveedores precisos, lo que permite a los beneficiarios de Medicare identificar y localizar a los proveedores. Por lo tanto, los CMS recomiendan a todos los proveedores mantener sus datos de Identificador Nacional de Proveedores (NPI) actualizados en el Sistema Nacional de Enumeración de Planes y Proveedores (NPPES).
Ediciones médicamente improbables (MUE) - Actualización del sistema de edición de reclamaciones y recordatorio de facturación
- CHIP
- EPO
- FEP PPO
- HMO
- Medicare Advantage HMO
- POS
- PPO
- Tradicional e Integral
- Medicare Advantage PPO
PUNTO CLAVE: Capital está implementando actualizaciones del sistema para garantizar que las MUE se apliquen de manera consistente y precisa en todos los tipos de proveedores. Estas mejoras corrigen las brechas identificadas y alinean nuestro proceso según lo comunicado en boletines administrativos anteriores*.
Una MUE para un código HCPCS/CPT es el máximo de unidades de servicio que un proveedor informaría en la mayoría de las circunstancias para un único beneficiario en una única fecha de servicio.
Hay tres (3) tipos de Indicadores de adjudicación de MUE (MAI)
- MAI 1 - Límite de MUE aplicado a nivel de línea de reclamación. El uso adecuado de los modificadores permitirá informar unidades de servicio médicamente necesarias que excedan el límite de MUE.
- MAI 2 - Límite de MUE aplicado según la fecha de servicio. CMS no ha identificado ningún caso en el que sea pagadero un valor superior.
- MAI 3 - Límite de MUE aplicado según la fecha de servicio. En circunstancias raras o inusuales, se puede considerar el reembolso de unidades adicionales. Estas denegaciones de MUE pueden ser apeladas con documentación de respaldo.
Límites de MUE aplicados a nivel de línea de reclamación (MAI 1)
Cuando las unidades de servicio excedan el valor de MUE, informe lo siguiente:
- Las unidades reportadas en cada línea no deben exceder el límite.
- Al facturar varias líneas por el mismo servicio, anexe modificadores como 76, 77, 91, RT o LT, según corresponda.
Las líneas de reclamación con unidades que superen el valor de MUE no son elegibles para el pago.
Correcto |
Incorrecto |
|---|---|
|
Línea 1 - Procedimiento J7214, 7500 unidades. (La línea MUE es 7500) Línea 2 - Procedimiento J7214, 756 unidades. (El exceso de unidades será elegible para el pago) |
Línea 1 - Procedimiento J7214, 8256 unidades. (Denegará todas las unidades) |
Límites de MUE aplicados según la fecha de servicio (MAI 2 o 3)
Al informar unidades de servicio para la misma fecha que excedan el valor de MUE, informe lo siguiente:
- Informe unidades hasta el límite de MUE en una línea.
- Informe unidades que excedan el valor de MUE en la línea siguiente.
Esto permite que las unidades de servicio hasta el valor MUE sean elegibles para el pago.
Correcto |
Incorrecto |
|---|---|
|
Línea 1 - Procedimiento J1568, 300 unidades. (MUE es 300) Línea 2 - Procedimiento J1568, 20 unidades. (El exceso de unidades se denegará) |
Línea 1 - Procedimiento J1568, 320 unidades. (Denegará todas las unidades) |
Referencias:
FP 01.001 Metodología de codificación y reembolso correcta
Boletín administrativo: 2022-06-001
Boletín administrativo: 2022-12-001
Boletín administrativo: 2025-05-002
Exámenes de diagnóstico de cáncer de mama
- CHIP
- EPO
- FEP PPO
- HMO
- Medicare Advantage HMO
- POS
- PPO
- Tradicional e Integral
- Medicare Advantage PPO
PUNTO CLAVE: Este boletín proporciona orientación sobre estudios por imágenes adicionales cubiertos como preventivos cuando se recomienda completar el proceso de exámenes de diagnóstico preventivos del cáncer de mama o abordar hallazgos identificados en la mamografía preventiva inicial.
De acuerdo con los mandatos estatales y federales, la cobertura preventiva de Capital Blue Cross incluye exámenes mamográficos para personas cubiertas de 40 años o más (y para menores de 40 años cuando lo recomiende su médico).
Para las mujeres con riesgo promedio de cáncer de mama, la cobertura preventiva también incluye estudios por imágenes adicionales —como mamografía, resonancia magnética e ultrasonido— y, a partir del 1 de enero de 2026, evaluación patológica (biopsia), cuando se recomiende completar el proceso de exámenes de diagnóstico preventivos o abordar hallazgos identificados en el examen preventivo inicial.
Los proveedores deben cerciorarse de que todos los servicios adicionales de exámenes de diagnóstico y cualquier evaluación patológica realizada como parte del examen preventivo inicial del cáncer de mama para determinar malignidad se facturen como preventivos hasta que se establezca un diagnóstico.
Además, a partir del 1 de enero de 2026, para los exámenes de diagnóstico de cáncer de mama y de cuello uterino, la cobertura incluirá servicios de orientación al paciente y seguimiento, cuando corresponda, para respaldar el cumplimiento de las recomendaciones de exámenes de diagnóstico según la necesidad evaluada de apoyo de orientación del paciente.
Se recomienda a los proveedores revisar las Pautas de cobertura de salud para servicios preventivos, disponibles en "Educación y manuales" dentro de la biblioteca para proveedores en nuestro portal web para proveedores, para cerciorarse de que se reciban los servicios preventivos elegibles sin costos compartidos, cuando corresponda.
Orientación sobre recursos adicionales:
Solo proveedores profesionales
Certificación de CAQH - Recordatorio
- CHIP
- EPO
- FEP PPO
- HMO
- Medicare Advantage HMO
- POS
- PPO
- Tradicional e Integral
- Medicare Advantage PPO
PUNTO CLAVE: Los proveedores deben asegurarse de que su solicitud ante el Consejo de Atención Médica de Calidad Asequible (CAQH, por sus siglas en inglés) se actualice al menos cada 120 días.
Los proveedores pueden cumplir con la normativa de la siguiente manera:
- Revisando su solicitud de CAQH regularmente.
- Garantizando que toda la información esté actualizada y sea precisa.
- Completando el proceso de recertificación cada 120 días calendario.
Si no se vuelve a certificar dentro del plazo de 120 días, se pueden producir retrasos en la acreditación, la contratación y/o la participación en la red.
Para obtener más información, visite CAQH para proveedores o llame al 888.600.9802. Agradecemos enormemente su cooperación en el cumplimiento de este requisito.
Requisitos de facturación e informe de unidades de factores de coagulación para la hemofilia: actualizaciones del sistema de edición de reclamaciones
- CHIP
- EPO
- FEP PPO
- HMO
- Medicare Advantage HMO
- POS
- PPO
- Tradicional e Integral
- Medicare Advantage PPO
PUNTO CLAVE: A partir del 1 de junio de 2026, Capital mejorará nuestro sistema de edición de reclamaciones para respaldar mejor la aplicación de pautas de codificación correctas para productos con factor de hemofilia.
Se recuerda a los proveedores cerciorarse de que la cantidad facturada (QB) refleje con precisión el número de unidades internacionales (IU), miligramos (mg) o microgramos (mcg) administrados, según se define en el descriptor del código HCPCS.
Después de la conversión de la dosis administrada en unidades facturables, se deben evaluar las reclamaciones para garantizar el cumplimiento de las pautas de codificación correctas. Se requieren varias líneas de reclamación cuando:
- Las unidades de servicio exceden el límite de MUE a nivel de línea (MAI 1) asignado a ese código HCPCS, o
- Las unidades superan el máximo del sistema de 9,999 unidades por línea de reclamación.
Para el mismo código HCPCS y la misma fecha de servicio, ninguna línea de reclamación puede exceder el límite de MUE o el límite máximo del sistema de 9,999 unidades. Si el total de unidades supera cualquiera de los límites, las unidades deben dividirse y facturarse en varias líneas de reclamación, siguiendo todas las reglas de codificación y modificadores aplicables.
Límites de MUE aplicados a nivel de línea de reclamación (MAI 1)
Cuando las unidades de servicio excedan el valor de MUE, informe lo siguiente:
- Las unidades reportadas en cada línea no deben exceder el límite.
- Al facturar varias líneas por el mismo servicio, anexe modificadores como 76, 77, 91, RT o LT, según corresponda.
Las líneas de reclamación con unidades que superen el valor de MUE no son elegibles para el pago.
Ejemplo:
J7214 (Inyección, complejo de factor VIII/factor von Willebrand) tiene una MUE de 7500 unidades por línea de reclamación.
Correcto |
Incorrecto |
|---|---|
|
Línea 1 - Procedimiento J7214, 7500 unidades. (La línea MUE es 7500) Línea 2 - Procedimiento J7214, 756 unidades. (El exceso de unidades será elegible para el pago) |
Línea 1 - Procedimiento J7214, 8256 unidades. (Denegará todas las unidades) |
Para obtener detalles sobre FP 01.001 - Metodología de codificación correcta y reembolso, consulte las Políticas de reembolso de Capital.
Hay información adicional disponible a través de la Tabla de MUE de servicios para profesionales de CMS.
Nuevos graduados que solicitan unirse a la red
- CHIP
- EPO
- FEP PPO
- HMO
- Medicare Advantage HMO
- POS
- PPO
- Tradicional e Integral
- Medicare Advantage PPO
PUNTO CLAVE: Requisitos para los nuevos graduados que solicitan unirse a la red de Capital Blue Cross.
Todos los nuevos graduados deben haber completado toda su educación de posgrado antes de presentar su solicitud para unirse a la red. Además, los proveedores también deben haber recibido privilegios de admisión en al menos un hospital participante designado como su centro de admisión principal (para médicos que admiten pacientes) o tener otros acuerdos de hospitalización que hayan sido aprobados por Capital Blue Cross antes de enviar su solicitud para unirse a la red.
Los médicos que no están obligados a tener privilegios hospitalarios de admisión son anestesiólogos, alergólogos, médicos de sala de emergencias, dermatólogos, patólogos y radiólogos.
Solo proveedores de centros
Notificación de admisiones urgentes y de emergencia
- CHIP
- EPO
- FEP PPO
- HMO
- Medicare Advantage HMO
- POS
- PPO
- Tradicional e Integral
- Medicare Advantage PPO
PUNTO CLAVE: Se recuerda a los proveedores que notifiquen a Capital Blue Cross dentro de los plazos correspondientes las admisiones hospitalarias urgentes y/o de emergencia.
Las admisiones hospitalarias urgentes y/o de emergencia requieren notificación a Capital dentro de 2 días hábiles a partir de la admisión. La falta de notificación a Capital puede dar lugar a una denegación.
Puede encontrar más información en el Manual para Proveedores de Capital Blue Cross, Capítulo 5, Unidad 1 - Revisión concurrente.